Nebenwirkungen eines Beta-Rezeptorblockers können zu Beginn, aber auch zu einem späteren Zeitpunkt der Behandlung auftreten. Hier erfahren Sie mehr zu Nebenwirkungen und Feineinstellung einer Behandlung mit einem Beta-Blocker.

Beta-Rezeptorenblocker gehören zur Standardtherapie zur Behandlung von Herz-Kreislauf-Erkrankungen, zum Beispiel von Bluthochdruck, Herzrhythmusstörungen, Herzschwäche und Koronarer Herzkrankheit. Die Wirksamkeit auf Symptome der einzelnen Erkrankungen und ein positiver Einfluss auf das Langzeitüberleben sind zum Teil wissenschaftlich sehr gut belegt.
Beta-Rezeptorenblocker haben allerdings auch symptomatische Nebenwirkungen, die häufig als Folge der Behandlung mit Beta-Rezeptorenblocker nicht erkannt werden, was wiederum meistens den unnötigen zusätzlichen Einsatz von anderen Medikamenten nach sich zieht.
Die Behandlung mit einem Beta-Blocker verlangt ein besonderes Fingerspitzengefühl, um einen ausbalancierten Kreislauf ohne Nebenwirkungen zu erzielen.
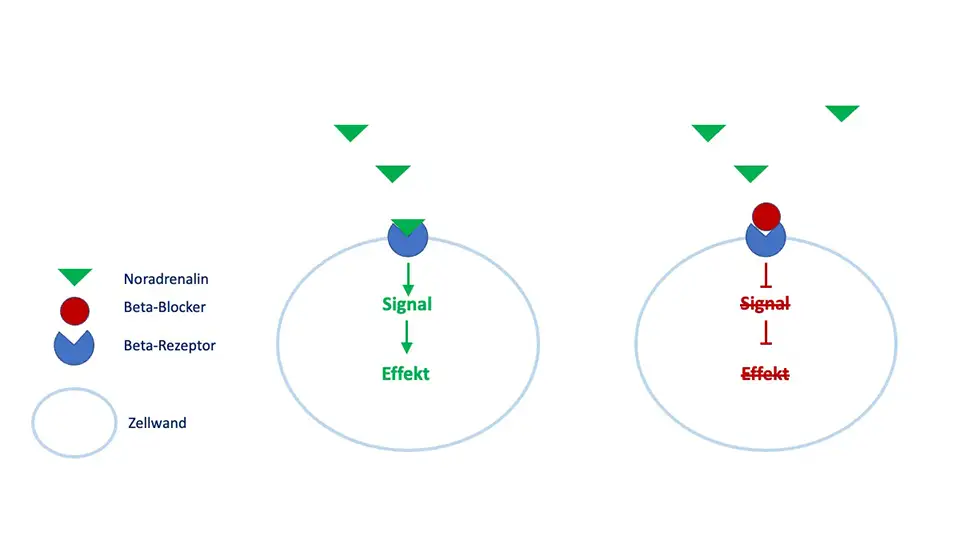
Beta-Rezeptorenblocker – Wirkmechanismus über Zellrezeptoren
Beta-Rezeptorenblocker blockieren Rezeptoren auf der Zelloberfläche, die die Wirkung von Noradrenalin und Adrenalin vermitteln. Noradrenalin und Adrenalin sind wesentliche Vermittler des „Fight-or-Flight“-Mechanismus und aktivieren folglich Ihren Körper; sie gehören vereinfacht gesagt zu den „Stresshormonen“.
Wir kennen unterschiedliche Beta-Rezeptoren, die in Körpergeweben unterschiedlich verteilt sind:
- Beta-1-Rezeptoren (Herz)
- Beta-2-Rezeptoren (Bronchien, Gebärmutter, Blutgefäße, Muskulatur)
- Beta-3-Rezeptoren (braunes, beiges und weißes Fettgewebe)
Beta-Rezeptorenblocker in der Herz-Kreislaufmedizin
In der Herz-Kreislaufmedizin werden überwiegend sogenannte selektive Beta-1-Rezeptorblocker eingesetzt, zum Beispiel Metoprolol, Bisoprolol, Nebivolol. Am Herz wirken sie wesentlich über folgende Mechanismen:
- elektrische Erregungsbildung und -leitung
- Pumpkraft
- Sogkraft
Die Wirkung auf die Erregungsbildung und -leitung bedeutet in erster Linie, dass Ihr Herz bei einer Beta-Blockertherapie in Ruhe und bei Belastung langsamer schlägt, was mit einem verringerten Sauerstoffverbrauch des Herzens einhergeht. Darüber hinaus werden Herzrhythmusstörungen, die durch Noradrenalin und Adrenalin vermittelt werden, zum Teil unterdrückt.
Die Pumpkraft des Herzens wird durch Beta-Blocker verringert, indem die Herzmuskelzellen sich weniger zusammenziehen können. Dieser Mechanismus reduziert wesentlich den Blutdruck, vor allen Dingen den oberen systolischen Wert.
Eng mit der Pumpkraft ist die Sogkraft des Herzens verknüpft. Das Herz ist eine Druck-Saugpumpe. Der Sog entsteht durch die Herzspitzenwärtsbewegung in der Auswurfphase der Hauptkammern. Während die Hauptkammern das Blut in den nachgeschalteten Kreislauf pumpen, wird gleichzeitig Blut aus dem vorgeschalteten Kreislauf in die Vorkammern eingesaugt. Beta-Rezeptorenblocker bewirken, dass weniger Blut angesaugt wird, so dass es im vorgeschalteten Gewebe, vor dem rechten Herzanteil in den Beinen und vor dem linken Herz in der Lunge zu Flüssigkeitsansammlungen, den sogenannten Ödemen kommen kann.
Die Beta-1-Rezeptorenblocker gelten als selektiv, das heißt, sie sollten nur auf Beta-1-Rezeptoren des Herzens wirken. Das ist aber in der Realität nicht ausschließlich so, weil a) eine Kreuzreaktion mit Beta-2- und Beta-3-Rezeptoren besteht, das heißt, dass auch diese Rezeptoren, wenn auch schwächer blockiert werden können und b) Beta-1-Rezeptoren auch in anderen Geweben vorhanden sind, zum Beispiel in der Zirbeldrüse im Gehirn (Melatoninfreisetzung).
Nebenwirkungen durch Beta-Rezeptorenblocker
Symptome sind ein erster und wichtiger Hinweis für die Nebenwirkung von Beta-Rezeptorenblockern, die dann mithilfe von apparativen Methoden weiter abgeklärt werden müssen.
Symptome durch Beta-Rezeptorenblocker
Einige symptomatische Nebenwirkungen einer Behandlung mit Beta-Rezeptorenblockern lassen sich wie folgt zusammenfassen:
- Herz
- langsame Herzfrequenz in Ruhe (<50 bpm)
- Herzfrequenz bei Belastung nicht >100
- niedriger Blutdruck
- hoher systolischer Blutdruck (paradox, bei niedriger Herzfrequenz)
- Wasser in den Beinen (Beinödeme)
- Kreislauf
- Gesichtsblässe in Ruhe mit Verschwinden beim Sprechen oder Lachen
- kalte Füße und Hände
- Leistungseinschränkung bei Belastung
- Lunge
- Luftnot durch Engstellung der Bronchien
- Luftnot durch Wasseransammlung in der Lunge
- Stoffwechsel
- Muskelschwäche
- Kältegefühl
- Gewichtszunahme
- Gehirn
- Müdigkeit
- Antriebsarmut
- Schlafstörungen
Zeitpunkt des Auftretens von Nebenwirkungen der Beta-Rezeptorenblockertherapie
Die Nebenwirkungen von Beta-Rezeptorenblockern können zu jedem Zeitpunkt der Therapie auftreten, auch erst nach Jahren.
Am Anfang der Behandlung ist es häufig eine Überdosierung, die die Symptome verursacht. Im Verlauf der Zeit kann sich das Gleichgewicht zugunsten des Parasympathikus, des beruhigenden Anteils des vegetativen Nervensystems verschieben, zum Beispiel durch weniger Stress bei Arbeit, Behebung von Schlafstörungen oder Sport. Dann können Beta-Blocker relativ überdosiert sein und die Nebenwirkungen treten dann erst hervor.
Je älter wir werden, desto geringer ist der Bedarf an Betablockern und die Dosis muss fast immer mit den Jahren nach unten angepasst werden.
Sonderfall – Beta-Blockertherapie nach Herzoperation
Ein besonderer Fall ist der Zustand nach einer Herzoperation, zum Beispiel einer aorto-koronaren Bypassoperation oder einer Herzklappenoperation.
Bei den meisten Herzoperation eröffnen die Herzchirurgen über dem rechten Herzen den umgebenden Herzbeutel, um an das Herz zu gelangen. Mit Beendigung der Operation wird der Herzbeutel meistens nicht wieder verschlossen, sodass der Herzbeutel bei einer Schwellung des Herzmuskels in der unmittelbaren post-operativen Phase das Herz nicht einengt. Eigentlich ist dieses Vorgehen heutzutage aufgrund neuer Methoden (moderne Kardiologie-Lösung) nicht mehr erforderlich, wird aber weiter praktiziert, nicht zuletzt, weil die Langzeitfolgen nicht bekannt sind.
In der unmittelbaren post-operativen Phase sind das Herz und der Gesamtorganismus als Teil des Heilungsprozesses entzündlich aktiviert und damit ist auch das Risiko für Herzrhythmusstörungen gesteigert, was den Einsatz auch von höheren Dosierungen von Betablockern über einige Wochen rechtfertigt.
Allerdings beruhigt sich die Gesamtsituation zunehmend und gleichzeitig kommt es zu sogenannten rechtsventrikulär-perikardialen Adhäsionen, das heißt einer Verklebung zwischen rechtem Herzmuskel und Herzbeutel. Das hat zur Folge, dass die Sogkraft des rechten Herzmuskels um bis zu 50% gemessen an der Herzspitzabwärtsbewegung der rechten Hauptkammer reduziert sein kann. Die nicht-adäquate Behandlung mit einem Beta-Blocker kann dann in der späteren Phase nach der Operation mit erheblichen Nebenwirkungen verbunden sein, so zum Beispiel mit körperlicher Leistungseinschränkung, Müdigkeit und Beinödemen.
Sonderfall – Beta-Blockertherapie und Beinödeme
Menschen gehen häufig wegen Beinödemen, den sogenannten „dicken Beinen“ zum Arzt. Typisch ist, dass die Beine am Morgen schlank und am Abend geschwollen sind. Die Ursachen hierfür können vielfältig sein:
- zu geringe körperliche Aktivität
- schwache Beinmuskulatur
- Beinvenenschwäche
- Beckenbodenmuskelschwäche
- Herzschwäche
- Herzklappenfehler
- erhöhter Lungenarteriendruck
- Lungenüberblähung
- Medikamente (vor allen Dingen Calciumantagonisten, Beta-Rezeptorenblocker)
Bei einem Großteil der Ursachen für Beinödeme handelt es sich um die Folge eines gestörten venösen Rückstroms gegen die Schwerkraft, das heißt Flüssigkeit bleibt in den Beinen „hängen“, anstatt ins arterielle Gefäßsystem weitergeleitet zu werden. Dieses entspricht einer Umverteilungsstörung.
Nach Ausschluss einer relevanten Herz- und Lungenerkrankung wird unabhängig von weiteren Ursachen meist mit harntreibenden Medikamenten behandelt, anstatt die eigentlichen Ursachen zu beheben. Das hat zur Folge, dass zwar die Beine schlanker werden, allerdings wird auch dem Gesamtorganismus und hier vor allen Dingen dem Blutgefäßsystem Flüssigkeit entzogen, was wiederum Ihre Leistungsfähigkeit einschränkt.
Häufig genug ist die Behandlung mit einem Beta-Rezeptorenblocker und die damit verbundene Einschränkung der Sogkraft des Herzens eine wesentliche Ursache für Beinödeme. Falls Sie folglich Beinödeme aufweisen und gleichzeitig einen Beta-Rezeptorenblocker einnehmen, dann sollten Sie gemeinsam mit Ihrem Arzt oder Ihrer Ärztin die medikamentöse Therapie überprüfen und gegebenenfalls eine Feineinstellung der Beta-Blockertherapie vornehmen.
Beta-Rezeptorenblocker Abklärung von Nebenwirkungen und medikamentöse Feineinstellung
Für eine umfassende Abklärung möglicher Nebenwirkungen einer Therapie mit Beta-Rezeptorenblocker bewerten wir in der Cardiopraxis® folgende Punkte:
- Symptome
- Durchmesser der unteren Hohlvene in Rückenlage und im Stehen (Sonografie)
- Herzspitzenwärtsbewegung der rechten und der linken Herzhauptkammer (Gewebedoppler im Herzultraschall)
- Weite der Atemwege (Spirometrie)
- Kraft der Atemmuskulatur (Spiromanometrie)
- Herzfrequenz und Blutdruck unter Belastung (Fahrradergometrie)
- Blutflussmessung in Rückenlage und im Stehen (Photoplethysmografie)
- Drucksteigerung durch reflektierte Druckwellen (Arteriografie)
- Körpertemperatur und Temperaturempfinden
Zentral bei der Bewertung von Nebenwirkungen einer Beta-Blockertherapie sind die Bestimmung des Durchmessers der unteren Hohlvene, der Herzspitzenwärtsbewegung und die Herzfrequenz unter Belastung.
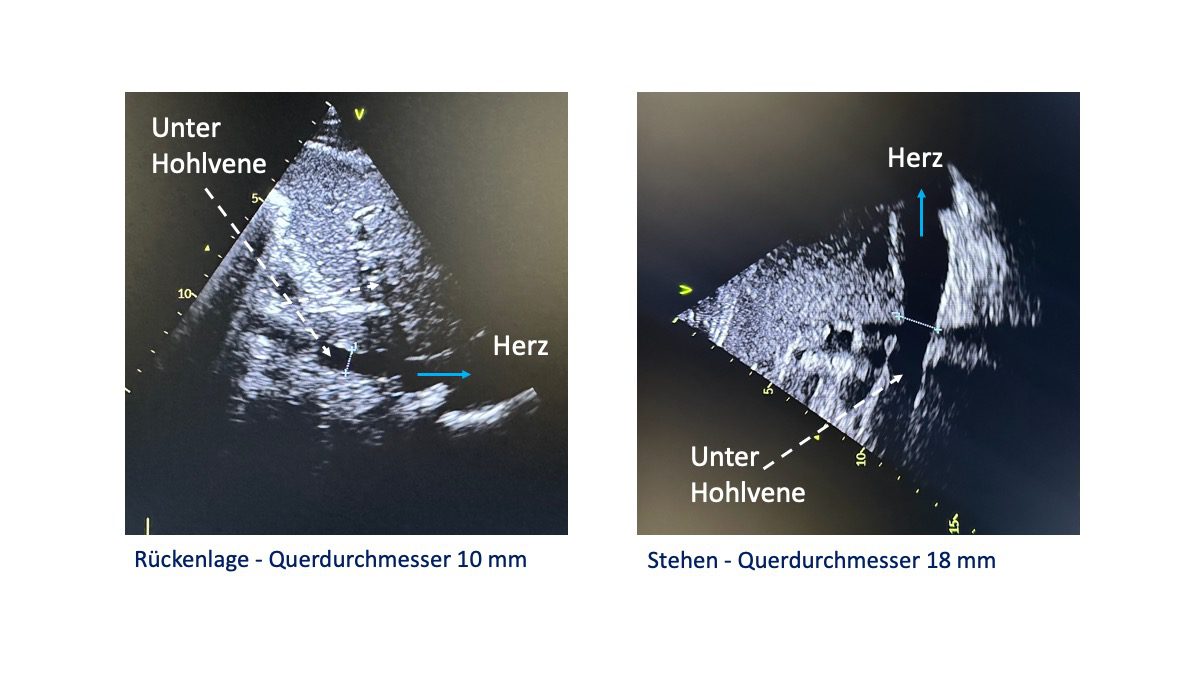
Durchmesser der unteren Hohlvene bei Nebenwirkung einer Beta-Blockertherapie
Der Durchmesser der unteren Hohlvene, der Vena cava ist ein indirektes Mass für den Flüssigkeitsgehalt im venösen Blutgefäßsystem. Von der Rückenlage zum Stehen nimmt der Diameter den Vena cava normalerweise ab oder bleibt konstant, weil venöses Blut bedingt durch die Schwerkraft die Tendenz hat in den tieferen Gefäßabschnitten, zum Beispiel den Beckenvenen zu verbleiben und gleichzeitig bedingt durch Sogkraft von Lunge und Herz Blut in den Brustraum gesogen wird.
Ist der Durchmesser der Vena cava unter Berücksichtigung der Körpergröße in Rückenlage zu weit, zum Beispiel >18 mm und nimmt der Durchmesser im Stehen zu, zum Beispiel auf 20 mm, dann ist dieses ein eindeutiger Hinweis auf eine nachgeschaltete venöse Abflussstörung, eine sogenannte rechts-kardiale Einflussstauung. Ursachen für eine rechts-kardiale Einflussstauung sind im Wesentlichen:
- eingeschränkte Atemmuskelkraft
- Herzklappenfunktionsstörungen (zum Beispiel Trikuspidalklappeninsuffizienz des rechten Herzens)
- erhöhter Blutgefäßwiderstand der nachgeschalteten arteriellen Gefäßsysteme (pulmonal-arterieller und systemarterieller Kreislauf)
- strukturelle Herzmuskelschwäche (zum Beispiel nach Herzinfarkt)
- medikamentös-induzierte Herzschwäche (zum Beispiel Betablocker)
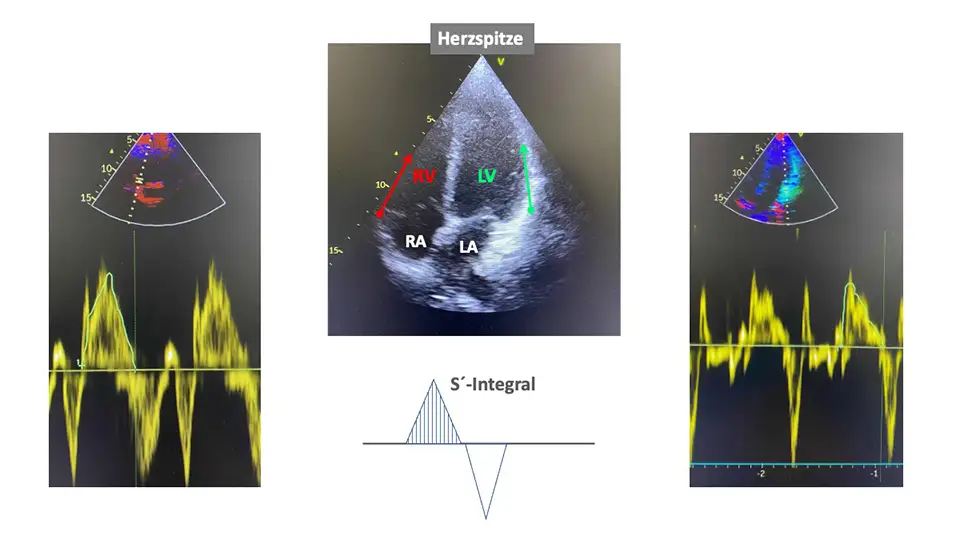
Sogkraft des Herzens bei Nebenwirkung einer Beta-Blockertherapie
Sowohl der rechte als auch der linke Herzanteil sind eine Druck-Saugpumpe. Während die jeweiligen Hauptkammern Blut als Schlagvolumen in den nachgeschalteten Kreislauf auswerfen, füllen sich bei geschlossenen Verbindungsklappen zwischen Vor- und Hauptkammern (Trikuspidal- bzw. Mitralklappe) die Vorkammern durch einen Sog, der durch die Bewegung des Herzens zu herzspitzenwärts. Das ist ähnlich dem Prinzip einer Melkbewegung beim Melken einer Kuh.
Die Herzspitzenwärtsbewegung lässt sich als „Sogkraft“ mit dem sogenannten Tissue-Doppler im Herzultraschall sehr zuverlässig bestimmen. Dabei wird ein Messvolumen auf die Seitenwand der jeweiligen Hauptkammer gelegt und die Geschwindigkeit der Auslenkung der Herzkammer zur Herzspitze in cm/sec bestimmt. Die normalen Geschwindigkeiten betragen hier >10 cm/sec.
Zur Bestimmung der Sogkraft ziehen wir das Integral, das heißt den mittleren Wert während einer Aktion heran. Die Referenzwerte liegen bei:
- rechte Hauptkammer: 3,0-3,5 cm/sec
- linke Hauptkammer: 2,0-2,5 cm/sec
Wird der untere Grenzwert unterschritten, dann ist das ein sicherer Hinweis auf eine eingeschränkte Sogkraft. Besteht gleichzeitig eine Behandlung mit einem Beta-Blocker, dann können wir zumindest von einer relevanten Teilverursachung des Beta-Blockers ausgehen. Der Vollständigkeit halber sei hier erwähnt, dass kardiotrope Calciumantagonisten, wie Verapamil und Diltiazem, welche heute nur noch selten verordnet werden, ebenfalls zu diesem Phänomen führen können.
Herzfrequenz unter Belastung bei Nebenwirkung einer Beta-Blockertherapie
Wenn Sie sich körperlich belasten, dann muss auch das zirkulierende Blutvolumen erhöht werden, um die Arbeitsmuskulatur mit Nährstoffen zu versorgen und Abfallstoffe abzuführen. Ihr Herz trägt dazu über 2 Mechanismen bei, es pumpt kräftiger und schneller. Bis zu einer Herzfrequenz von circa 100 bpm greifen beide Mechanismen. Da sich die Herzhauptkammern während der Auswurfphase aber nie komplett entleeren können, ist es ab einer Herzfrequenz von 100 bpm so, dass lediglich die Herzfrequenz zu einer Steigerung des sogenannten Herzzeitvolumens beiträgt.
Der Beta-Blocker führt zu einer Drosselung, einer sogenannten chronotropen Inkompetenz. Diese können wir in der Fahrradergometrie sehr gut erfassen und dann die Medikation entsprechend anpassen.
Medikamentöse Feineinstellung der Beta-Blockertherapie
Die Behandlung mit Beta-Blockern ist und bleibt ein wertvoller Bestandteil der Behandlung von Herz-Kreislauferkrankungen. Die Feineinstellung der Dosis ist es, welche zu Beginn aber auch im Verlauf der Behandlung bei Auftreten von Nebenwirkungen eine Herausforderung darstellt.
Messwerte erhoben mit den oben genannten Methoden sind neben den Symptomen die unabdingbare Richtschnur für eine optimale Einstellung. Die Messwerte müssen nach medikamentöser Umstellung entsprechend kontrolliert werden, in der Regel nach zwei Wochen.
Einschränkung der körperlichen und geistigen Leistungsfähigkeit durch Beta-Blocker – medikamentöse Anpassung
Grundsätzlich sollte bei Einschränkungen der körperlichen und geistigen Leistungsfähigkeit an eine Nebenwirkung der Beta-Blockertherapie gedacht werden. Neben den Symptomen dienen hier die maximale Herzfrequenz unter Belastung und der Durchmesser der Vena cava inferior als Orientierung bei der Feineinstellung.
Liegt die maximale Belastungsherzfrequenz bei ≤ 100 bpm, dann reduzieren wir den Betablocker schrittweise so lange bis eine maximale Herzfrequenz von 120 bpm möglich wird, was ungefähr dem aeroben Belastungsbereich entspricht und für die Erledigung von Alltagsaktivitäten vollkommen ausreichend ist. In hohem Lebensalter sind auch niedrigere maximale Herzfrequenzen individuell möglich.
Eine Weitstellung der unteren Hohlvene signalisiert eine vermehrte Dehnung der Vene selbst, aber auch indirekt der Herzvorkammern. Dieses wiederum ist zum Schutz vor Überdehnung mit einer Aktivierung des Parasympathikus verbunden, was Müdigkeit und Antriebslosigkeit als Nebenwirkung erklären kann. Hier achten wir bei der Reduktion darauf, dass der Diameter der Hohlvene sowohl in Rückenlage als auch im Stehen abnimmt.
Bluthochdruck – Feineinstellung der Betablockertherapie
Treten bei der Behandlung des Bluthochdrucks messbar verifizierte Nebenwirkungen des Beta-Blockers auf, dann reduzieren wir den Betablocker schrittweise. Gerade bei einer Ruheherzfrequenz von <64 bpm ist das erfolgversprechend, weil in bei niedrigen Herzfrequenzen der systolische Blutdruck durch reflektierte Druckwellen erhöht sein kann; Ziel ist eine Herzfrequenz von circa 72 bpm.
Zusätzlich nutzen wir in der Cardiopraxis die nicht-invasive Blutflussmessung des Kreislaufs und streben dabei einen Ruhewert von 100-135% des unteren Grenzwertes von 2,2 Liter pro Minute pro m2 Körperoberfläche in Ruhe an.
Falls der Blutdruck unter Reduktion des Betablockers ansteigt, nutzen wir andere Medikamente, die den Blutdruck senken, zum Beispiel die Steigerung einer Behandlung mit einem AT1-Blocker oder ACE-Hemmer.
Vorhofflimmern – optimale Frequenzkontrolle mit möglichst optimaler Dosierung eines Beta-Blockers
Häufig wird ein Betablocker zur Frequenzkontrolle, das heißt zur Verhinderung von zu hohen Herzfrequenzen bei permanentem Vorhofflimmern eingesetzt. Falls erforderlich kann der Beta-Blocker ganz oder zum Teil gegen ein Digitalispräparat, zum Beispiel Digoxin ausgetauscht werden. Die Kontrolle erfolgt hier mit einem Langzeit-EKG.
Herzschwäche – Dosis an Zielwerte anpassen
Beta-Blocker werden bei Herzschwäche eingesetzt, um das Herz vor einer Überstimulierung durch das sympathische Nervensystem (Noradrenalin, Adrenalin) zu schützen.
Das Gleichgewicht des Nervensystems zwischen Sympathikus („Gaspedal“) und Parasympathikus („Bremspedal“) kann über die Bestimmung des Durchmessers der unteren Hohlvene und der „Sogkraft“ im Herzultraschall die Feineinstellung erfolgen. Da aufgrund der zugrundeliegenden Herzschwäche normale Werte für die „Sogkraft“ meistens nicht erzielt werden können, ist eine Verringerung beziehungsweise ein Verschwinden der Symptome eine wichtige Richtgröße. Dabei kann es durchaus vorkommen, dass Beta-Blockerdosierungen von 6,25% der Maximaldosierung ausreichend sind.
Reduktion des Beta-Blockers und andere Medikamente
Wenn ein Beta-Blocker reduziert wird, dann wird das zirkulierende Blutvolumen gesteigert, was auch mit einer erhöhten Durchblutung der Niere und damit auch mit einer vermehrten Harnausscheidung verbunden ist. Hier besteht das Risiko, dass dem Körper zu viel Flüssigkeit entzogen wird, was mit Nebenwirkungen, wie zum Beispiel innerer Unruhe, erhöhter Herzfrequenz und sogar erhöhtem Blutdruck verbunden sein kann.
Bei einer Reduktion eines Beta-Blockers müssen wir daher auf einen ausgeglichenen Flüssigkeitshaushalt achten. Das bedeutet, dass harntreibende Medikamente, die sogenannten Diuretika gegebenenfalls gleichsinnig reduziert werden beziehungsweise die Trinkmenge angepasst wird. Auch dieses Vorgehen erfordert große ärztliche Sorgfalt bei der die Bestimmung des Durchmessers der unteren Hohlvene ein wertvoller Verlaufsparameter ist.
Risiken bei der Reduktion einer Beta-Blockertherapie
Da bei Reduktion einer Behandlung mit einem Beta-Blocker eine vermehrte Aktivität des Sympathikus zugelassen wird, müssen wir auf mögliche Nebenwirkungen achten. Hierzu zählen zum Beispiel:
- innere Unruhe
- erhöhte Herzfrequenz
- erhöhter Blutdruck
- Herzrhythmusstörungen
Ziel der Reduktion eines Beta-Blockers ist es daher die Nebenwirkungen des Betablockers zu reduzieren, ohne dass Nebenwirkungen der Reduktion auftreten. Dieses entspricht einem Gleichgewicht, was nur mit besonderer Sorgfalt und mit Hilfe von Messmethoden erzielt werden kann. Daher sollten Sie nie den Beta-Blocker ohne Abstimmung mit einem Arzt verringern, da Sie sonst auch Ihre Gesundheit gefährden könnten.
Literatur







